A Life Worth Living
Those who worked alongside famed transplant surgeon Thomas E. Starzl, MD, PhD, knew he regarded his young patients as the true heroes of his pioneering work at UPMC Children’s Hospital of Pittsburgh. Asked what he felt was his main contribution to the lives of children, Dr. Starzl simply replied, “letting them grow up.”
He focused on the long-term impact — to see his patients not just surviving, but thriving. When told of three- and five-year outcomes, he’d ask about 25-year outcomes.
At age 36, Renée Williams is living proof of his vision — thanks to a lifesaving liver transplant Dr. Starzl performed in 1985.
Surviving and Thriving
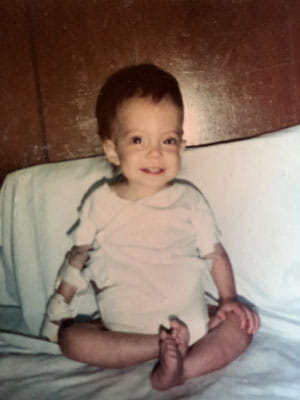 Renée was just 10 months old when diagnosed with alpha-1 antitrypsin deficiency (AADT) — an inherited condition caused by a defective gene that destroyed her liver. Four months later at UPMC Children’s Hospital, she received a remarkable gift from a Nebraska boy — a donated liver that saved her life and cured her disease.
Renée was just 10 months old when diagnosed with alpha-1 antitrypsin deficiency (AADT) — an inherited condition caused by a defective gene that destroyed her liver. Four months later at UPMC Children’s Hospital, she received a remarkable gift from a Nebraska boy — a donated liver that saved her life and cured her disease.
Thirty-five years later, Renée still has that liver, is in good health, and is flourishing as a corporate lawyer turned nonprofit executive and passionate volunteer. She was recently named executive director of the National Center for Victims of Crime in Washington, D.C.
“I’m very excited. I’m in a position to do amazing things on the forefront of issues such as victims’ rights and recovery, criminal justice reform, and human trafficking,” says Renée.
“I’m passionate about giving people help when they need help.”
Paying It Forward
Renée says she’s driven to “pay it forward” by gratitude for what she describes as her “fairy tale life.” She feels indebted — to the parents who made the difficult decision to donate their son’s liver after his death, to Dr. Starzl and his team at UPMC Children’s, and for the ongoing care she has received through UPMC’s transplant program.
“To whom much is given, much is expected. And I was given a whole heck of a lot,” says Renée. “I feel compelled to do things to give back.”
In 1985, Renée was a very sick little girl from Hubbard, Ohio, outside of Youngstown; the transplant changed everything. She grew up a “rough and tumble tomboy” with parents who were never overprotective.
“They listened when a doctor told them to treat me normal — not like I was going to die — or they’d be raising a monster,” she says.
By age 13, she weaned off the immunosuppressive drugs used to prevent rejection. She played sports, including volleyball and varsity golf, throughout middle school and high school. At age 16, she was volunteering in a local hospital.
Career of Service
 Renée began volunteering in Pittsburgh at UPMC Children’s while pursuing a theater degree at Point Park University.
Renée began volunteering in Pittsburgh at UPMC Children’s while pursuing a theater degree at Point Park University.
“I love Children’s — it’s like home to me. I knew how much it stunk to be in the hospital, and I wanted to do as much as I could to help other kids,” she says.
After a brief time working in Hollywood on the set of “The Young and the Restless,” Renée decided “on a whim” to pursue a career in law. She continued volunteering at UPMC Children’s while earning her law degree at the University of Pittsburgh.
Over the next 10 years, she offered comfort to patients at UPMC Children’s, mentored at-risk children through Big Brothers/Big Sisters, and worked with lower income families as an intern and volunteer at Christian Legal Aid of Pittsburgh. In 2012, Pittsburgh Magazine put her on their 40 Under 40 List in recognition of her volunteer work.
In 2015, after seven years as a corporate lawyer in the health care industry, Renée became executive director of Laurel Legal Services, a nonprofit providing free civil legal services to low income residents in southwestern Pennsylvania.
“I wanted to do more for people beyond volunteer work,” says Renée, explaining why she left corporate law. “I felt I had more talent and skills to give.”
In 2019, Renée moved to the nation’s capital, where she took the reins as director of another nonprofit — the National Crime Victim Bar Association, an affiliate of the National Center for Victims of Crime (NCVC). After just one year at the helm — and after a nationwide search — she became executive director of NCVC, a nonprofit organization dedicated to helping victims of crime rebuild their lives.
“I couldn’t pass it up. It was the chance to lead an organization committed to helping people, families, and communities harmed by crime,” she says.
Remembering Her Heroes
On March 11 as she celebrated her 36th birthday — two days after starting her new job — Renée thought of Dr. Starzl, whom she reconnected with in her 20s. The two became close friends and he even attended her law school graduation. They shared the same birthday and celebrated together when he turned 90 a year before his death in 2017.
She also thought of the little boy whose death enabled her to live and his family’s selfless gift. That night, she received another special gift — birthday wishes from the boy’s mother.
“It meant so much to hear from her,” says Renée.
“They both had such a tremendous impact on my life,” adds Renée. “They’re my heroes. I will be forever grateful to the donor family and to Dr. Starzl and my transplant family at Children’s Hospital.”









