- Find a Doctor
-
For Parents
- Before Your Visit
- During Your Visit
- After Your Visit
- More Resources for Parents
Patient & Visitor Resources -
Services
- Locations
-
About Us
- About Childrens
- Find it Fast
- Additional Resources
Find it FastAdditional Resources - MyCHP
ALERT:
There is construction in and around UPMC Children’s Hospital that is affecting the traffic flow – please allow for extra time traveling into the hospital.
- Find a Doctor
- For Parents
-
Services
-
Frequently Searched Services
- Asthma Center
- Brain Care Institute (Neurology & Neurosurgery)
- Cancer
- UPMC Children's Express Care
- Ear, Nose, & Throat (ENT)
- Emergency Medicine
- Endocrinology
- Gastroenterology
- Heart Institute
- Genetic & Genomic Medicine
- Infectious Diseases
- Nephrology
- Newborn Medicine
- Primary Care
- Pulmonary Medicine
- Rheumatology
- Surgery
- Transplant Programs
- See All Services
-
Frequently Searched Services
- Locations
- About Us
- MyCHP
- I Want To
- More Links









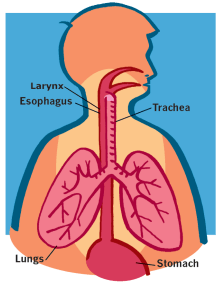 In a bronchoscopy (bron-KOS-ka-pee), a long flexible tube with a tiny camera, called a bronchoscope (BRONK-a-scope), is passed through the nose or mouth into the lungs. The doctor can see what the vocal cords, trachea (TRAKE-ee-uh) and the airways in the lungs look like.
In a bronchoscopy (bron-KOS-ka-pee), a long flexible tube with a tiny camera, called a bronchoscope (BRONK-a-scope), is passed through the nose or mouth into the lungs. The doctor can see what the vocal cords, trachea (TRAKE-ee-uh) and the airways in the lungs look like.
