Congenital diaphragmatic hernia (CDH) is a serious and complex birth defect. Every year, approximately 1,000 babies are born with CDH in the United States.
This condition affects multiple organ systems and requires long periods of care and follow up. For this reason, it is important that families seek help from a trusted, experienced, and specialized medical provider.
The Center for Congenital Diaphragmatic Hernia at UPMC Children's Hospital of Pittsburgh provides advanced care for this life-threatening condition. We have decades of experience in managing infants and children with CDH. Our skilled multidisciplinary team supports you and your baby before, during, and after birth — and beyond — close to home.
Learn more about:
Contact the Center for Congenital Diaphragmatic Hernia
Contact the Center for Congenital Diaphragmatic Hernia at UPMC Children's by phone at 412-692-7280 or by completing our online form.
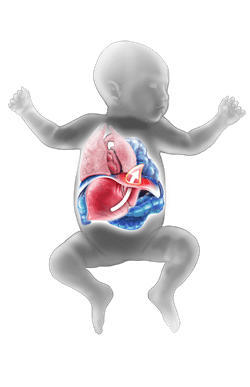
Congenital diaphragmatic hernia
The diaphragm is a thin sheet of muscle that divides the abdomen from the chest cavity. It plays a critical role in breathing. CDH is a birth defect that occurs when the diaphragm doesn't form properly in the womb. This creates a hole that allows abdominal organs to push, or herniate, into the chest. CDH can involve the:
- Stomach.
- Intestines.
- Spleen.
- Liver.
Although CDH can occur on either side of the chest, it occurs on the left side nearly 80% of the time. It rarely happens on both sides at the same time.
When abdominal organs move into the chest, they crowd the baby's heart and lungs. The most severe cases occur when the liver also moves into the chest. CDH leads to underdeveloped lungs and causes difficulty in breathing soon after birth.
The lungs of children affected with CDH have two main issues:
- Pulmonary hypoplasia: Small lungs, which affects the exchange of oxygen and carbon dioxide between the lungs and the bloodstream.
- Pulmonary hypertension: High blood pressure in the blood vessels of the lungs.
What causes CDH?
The exact cause of CDH is not known. Scientists believe it is due to genetics or possible environmental exposure during pregnancy. Most cases of CDH are isolated, meaning it is the baby's only major health problem. But some infants are born with other congenital anomalies, such as heart disease, or a genetic abnormality.
Back to top
Prenatal Diagnosis and Assessment of CDH
CDH is most often detected during a routine 20-week prenatal ultrasound. The test may show abdominal organs in the chest cavity where the lungs should be. The baby's heart also may be pushed to one side.
If an ultrasound indicates a potential CDH in your newborn, the medical team will initially refer you to our Fetal Diagnosis and Treatment Center (FDTC) located at UPMC Magee-Womens Hospital and in partnership with UPMC Children’s, to meet with a maternal-fetal medicine (MFM) specialist for further evaluation. MFM specialists are doctors with expertise in handling high-risk pregnancies and complex fetal conditions. UPMC Magee is nationally recognized for its comprehensive and pioneering maternal fetal medicine program.
Other diagnostic tests can include:
- A detailed anatomy ultrasound to view the chest and abdomen and estimate your baby's lung size.
- A fetal echocardiogram to evaluate your baby's heart structure and function.
- A fetal MRI to help evaluate the extent of the CDH, including the location of the liver.
These tests will be used to provide an accurate diagnosis. They can help doctors determine how severe the CDH is, identify associated conditions, and what kind of care your baby will need.
Management during pregnancy
UPMC Magee's MFM specialists will support you throughout your pregnancy. Care will also be provided by our neonatologists and pediatric surgeons at the Center for Congenital Diaphragmatic Hernia.
Once all tests are finished, the team of experts from UPMC Magee and UPMC Children's will meet with you to discuss the results. We answer your questions, provide support, and create a plan of care before, during, and after delivery. Other support may be provided by:
- Genetic counselors.
- Cardiologists.
- Fetal imaging experts.
During your pregnancy, we will check your baby's health regularly to prepare for their birth and care. We will monitor your baby's growth and well-being using ultrasound.
Other care options
Around half of the women and babies we treat at the Center receive referrals from their obstetrician or primary care doctor. Babies with CDH who are born at another hospital are transported directly to UPMC Children's Neonatal Intensive Care Unit (NICU) for care. The UPMC Children's Critical Care Transport team has the expertise needed to ensure the safe and timely transfer of babies to our NICU.
Nationwide, about 30% to 40% of CDH cases are not diagnosed until the baby is born. The defect is usually discovered when a newborn has trouble breathing immediately after birth. Other symptoms can include bluish discoloration from a lack of oxygen, a rapid heart rate, or a barrel-shaped chest. We provide immediate care for these newborns from throughout western Pennsylvania, Ohio, West Virginia, Maryland, and other locations.
Back to top
Delivery and Postnatal Treatment
Breathing support
Newborns with CDH have a high risk of severe breathing problems because their lungs are underdeveloped. Stabilizing breathing is the first and most important step in caring for these fragile newborns. Surgery to repair the CDH usually happens within a few days to a week after birth.
Babies with CDH at UPMC Magee are immediately moved to the hospital’s NICU (see our video introduction to the Neonatal Intensive Care Unit, below) for breathing support and lung protection.
- A breathing tube is inserted and the baby is placed on a ventilator.
- A tube is inserted into the stomach through the nose or mouth to prevent air build up that can cause pressure on the lungs.
- A technique called gentle ventilation is used to support breathing. This is done while monitoring and adjusting ventilator pressure to minimize any lung injury.
- Until the CDH is repaired, intravenous nutrition is provided.
- Special IVs are placed in the baby's umbilical cord, foot, or wrist.
Back to top
ECMO
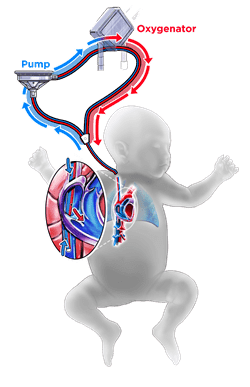 Newborns with severe breathing problems receive extracorporeal membrane oxygenation (ECMO) support. ECMO is a type of heart-lung bypass used for life-threatening heart and/or lung problems. It lets the baby's lungs and heart rest while a machine pumps blood and provides oxygen.
Newborns with severe breathing problems receive extracorporeal membrane oxygenation (ECMO) support. ECMO is a type of heart-lung bypass used for life-threatening heart and/or lung problems. It lets the baby's lungs and heart rest while a machine pumps blood and provides oxygen.
More about ECMO
Blood vessels in the lungs of babies with CDH are narrow due to pulmonary hypoplasia. ECMO bypasses these narrow blood vessels, providing cardiorespiratory support while the baby recovers.
Our dedicated ECMO-trained team is available 24/7 and includes an ECMO-credentialed neonatologist certified by the American Board of Pediatrics.
Ideally, your newborn should be weaned off ECMO support before surgery. In special cases, a decision may be made to repair the CDH while the baby remains on ECMO.
The Extracorporeal Life Support Organization recognizes UPMC Children's as a Platinum Center of Excellence in life support.
Additional Services
UPMC Magee and UPMC Children's Center for CDH also offer these services to support you and your baby:
- Prenatal diagnosis and counseling.
- Individualized care coordination and delivery planning.
- Postnatal surgical management.
- Long-term follow-up care.
- A highly trained family support team of pediatric doctors, nurses, social workers, and therapists.
- Chaplain support.
Back to top
Surgery for CDH
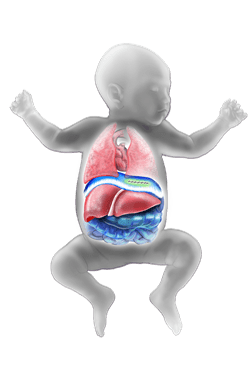
Congenital diaphragmatic hernia repair
UPMC Children's CDH Center offers years of pioneering expertise, a commitment to teamwork, and open communication with families. Our doctors have the skills and resources to respond quickly to any special circumstance. Our standardized clinical practice guidelines ensure consistent and high-quality care for all infants with CDH.
Our guidelines have led to:
- A reduced use of ECMO.
- An increased use of minimally invasive surgery.
- Outcomes that exceed national averages.
Newborns delivered at UPMC Magee receive care at the hospital's NICU until their breathing and other vitals are stable. Babies are then transferred to UPMC Children's Level 4 NICU for ongoing care and to prepare for CDH surgery. The timing of repair is carefully determined by our Center's medical and surgical teams based on your baby's case.
Our skilled pediatric surgeons will repair the defect in the diaphragm. They also will place the intestines and other organs back in the abdomen. More than half of all surgical repairs done by the Center are minimally invasive.
Different techniques are used to repair CDH based on the size of the hole and other factors. Small holes can be closed with stitches. Larger holes are closed using either a prosthetic patch or a muscle flap created from the baby's own tissue.
Other UPMC Children's specialists may be involved based on your baby's other care needs, including:
After surgery, your baby will need continued NICU care. Some infants may need nutritional support to help them grow and develop, such as a feeding tube. Continued oxygen support and medicine may also be needed to help with breathing.
Typical NICU stays are about 6 to 8 weeks. Recovery can take several months or longer for babies with severe CDH. Throughout your baby's NICU stay, you and your family are welcome members of our UPMC Children's family.
Back to top
Long-Term Outlook
Every baby with CDH is different. But advancements in medical care are continually improving long-term outcomes for even the most severe cases. While CDH is life-threatening, most newborns go on to recover. The best outcomes happen when newborns and children receive comprehensive, standardized, multidisciplinary care.
When your baby leaves UPMC Children's, our Center provides coordinated, ongoing outpatient care to support continued recovery. We can also connect your family to services and resources to help manage the stress and challenges of CDH.
Babies with CDH can face ongoing physical and developmental problems. These may include pulmonary hypertension, neurodevelopmental deficits, gastric reflux, and special nutritional needs. Our doctors, nurses, dietitians, nutritionists, and physical therapists will work with you and your baby. Together, we will identify, treat, and manage potential problems as early as possible.
In general, infants with mild CDH are regularly monitored until the age of 2, with additional checkups through age 5. Children with severe CDH may need ongoing care through late childhood or early adolescence.
Back to top
Why Choose the Center for Congenital Diaphragmatic Hernia at UPMC Children's?
- UPMC Children's is among a select group of pediatric hospitals with the expertise and resources to treat CDH. Our outcomes are among the best in the nation.
- We consistently rank as a top 10 children's hospital in the country by U.S. News & World Report. We also are ranked in the 10 pediatric specialties that are evaluated in U.S. News's annual survey. These include our programs in neonatology, cardiology, gastroenterology, and pulmonology. Access to such top-level medical/surgical expertise is important because babies and children with CDH often need years of care.
- Our Center's neonatologists and pediatric surgeons partner with maternal-fetal medicine experts at UPMC Magee-Womens Hospital to treat infants with CDH. UPMC Magee delivers nearly 10,000 babies each year.
- UPMC Children's Level 4 neonatal intensive care unit (NICU) provides 24/7 care for babies with complex CDH. Our NICU is staffed by skilled neonatologists, pediatric surgeons, respiratory therapists, and other specialists.
- We provide western Pennsylvania's only lifesaving extracorporeal membrane oxygenation (ECMO) for newborns. ECMO is an artificial heart and lung system often used to help support critically ill newborns, including, those with CDH.
- UPMC Children's is designated as a Platinum Level ELSO Center of Excellence. It is the highest level possible by the Extracorporeal Life Support Organization. This recognition acknowledges our expertise and commitment to providing advanced lifesaving support for infants and children.
- Our Center is engaged locally and nationally in research to advance the understanding and treatment of CDH, including:
Back to top












 Congenital diaphragmatic hernia
Congenital diaphragmatic hernia Newborns with severe breathing problems receive
Newborns with severe breathing problems receive  Congenital diaphragmatic hernia repair
Congenital diaphragmatic hernia repair