- Find a Doctor
-
For Parents
- Before Your Visit
- During Your Visit
- After Your Visit
- More Resources for Parents
Patient & Visitor Resources -
Services
- Locations
-
About Us
- About Childrens
- Find it Fast
- Additional Resources
Find it FastAdditional Resources - MyCHP
ALERT:
There is construction in and around UPMC Children’s Hospital that is affecting the traffic flow – please allow for extra time traveling into the hospital.
- Find a Doctor
- For Parents
-
Services
-
Frequently Searched Services
- Asthma Center
- Brain Care Institute (Neurology & Neurosurgery)
- Cancer
- UPMC Children's Express Care
- Ear, Nose, & Throat (ENT)
- Emergency Medicine
- Endocrinology
- Gastroenterology
- Heart Institute
- Genetic & Genomic Medicine
- Infectious Diseases
- Nephrology
- Newborn Medicine
- Primary Care
- Pulmonary Medicine
- Rheumatology
- Surgery
- Transplant Programs
- See All Services
-
Frequently Searched Services
- Locations
- About Us
- MyCHP
- I Want To
- More Links









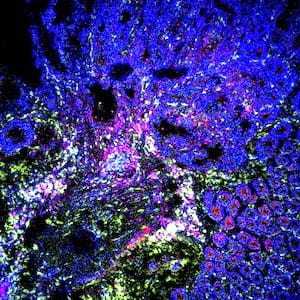 T cells at mucosal surfaces are critical to protection against invasive bacteria, viruses and parasites. However, if intestinal T cells become dysregulated, they can contribute to autoinflammatory diseases such as inflammatory bowel disease. We study how T cells in the small intestine and colon are shaped by the microbiome, both to the benefit and detriment of the host. We are interested in how interaction with specific micro-organisms can shape T cells to assist in vaccination and tumor immunotherapy. Alternatively, we are interested in how intestinal bacteria can shift T cells into inflammatory states, contributing to disease.
T cells at mucosal surfaces are critical to protection against invasive bacteria, viruses and parasites. However, if intestinal T cells become dysregulated, they can contribute to autoinflammatory diseases such as inflammatory bowel disease. We study how T cells in the small intestine and colon are shaped by the microbiome, both to the benefit and detriment of the host. We are interested in how interaction with specific micro-organisms can shape T cells to assist in vaccination and tumor immunotherapy. Alternatively, we are interested in how intestinal bacteria can shift T cells into inflammatory states, contributing to disease.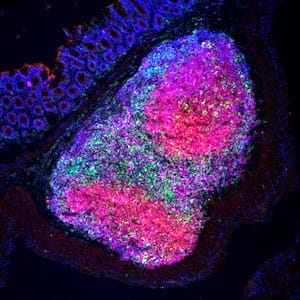 The immune system has a key role in the shaping of the microbiota. Maintaining homeostasis with regard to the microbiota is a lifelong process and shaped by the development of immunological memory against the bacteria that make up the microbiota. Infants are quickly colonized with bacteria that they have had no previous experience with and are therefore susceptible to both ineffective (leading to infection) and exaggerated (leading to damaging inflammation) immune responses against the microbiota. We hypothesize that one of the functions of maternal milk is to shape the developing microbiome towards health and that the primary mediators of that effort are antibodies, particularly Immunoglobulin A, secreted into the breast milk. This work has implications for many pediatric diseases and perhaps most notably necrotizing enterocolitis, where we have shown that disease is associated with a failure of IgA to bind to the bacteria present in the preterm intestine.
The immune system has a key role in the shaping of the microbiota. Maintaining homeostasis with regard to the microbiota is a lifelong process and shaped by the development of immunological memory against the bacteria that make up the microbiota. Infants are quickly colonized with bacteria that they have had no previous experience with and are therefore susceptible to both ineffective (leading to infection) and exaggerated (leading to damaging inflammation) immune responses against the microbiota. We hypothesize that one of the functions of maternal milk is to shape the developing microbiome towards health and that the primary mediators of that effort are antibodies, particularly Immunoglobulin A, secreted into the breast milk. This work has implications for many pediatric diseases and perhaps most notably necrotizing enterocolitis, where we have shown that disease is associated with a failure of IgA to bind to the bacteria present in the preterm intestine.